
Why we still haven’t stopped cholera
Why have attempts to get it under control failed? Rose George reports on an outbreak that went on far longer than anyone expected.

Parkin Parkin
UPDATE (August 2016): When we first published this story in July 2015, some people claimed that the United Nations was responsible for bringing cholera to Haiti in the 2010 outbreak – something that the organisation denied. However, in August 2016 the UN acknowledged that it played a role in the outbreak, which has since killed 10,000 people. You can read Mosaic’s shorter piece on the causes of the 2010 outbreak here.
In early February, when Jenniflore Abelard* arrived at her parents’ house high in the hills of Port-au-Prince, her father Johnson* was home. He was lying in the yard, under a tree, vomiting. When Jenniflore spoke to him, his responses, between retches, sounded strange: “nasal, like his voice was coming out of his nose”. He talked “like a zombie”. This is a powerful image to use in Haiti, where voodoo is practised and where the supernatural doesn’t seem as far-fetched as it might elsewhere. Her father’s eyes were sunk back into his head. She was shocked, but she knew what this was, because she has lived through the past five years in Haiti. She has lived through the time of kolera.
On 18 October 2010, Cuban medical brigades working in the areas around the town of Mirebalais in Haiti reported a worrying increase in patients with acute, watery diarrhoea and vomiting. There had been 61 cases the previous week, and on 18 October alone there were 28 new admissions and two deaths.
That was the beginning. Five years on, cholera has killed nearly 9,000 Haitians. More than 730,000 people have been infected. It is the worst outbreak of the disease, globally, in modern history. Hundreds of emergency and development workers have been working alongside the Haitian government for five years, trying to rid the country of cholera, and millions of dollars have been dispensed in the fight to eradicate it. But it’s still here. Why?
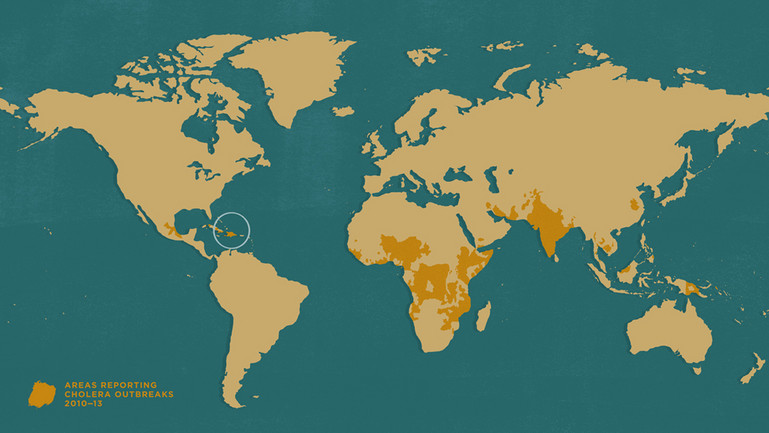
Areas reporting cholera outbreaks 2010–13. Based on information from WHO. Hispaniola, the island where Haiti is situated, is circled.
Parkin Parkin
In 1884, the scientist Robert Koch sent a dispatch from Kolkata to the German Interior Ministry about the bacterium that he had been studying. It was “a little bent, like a comma”, he wrote. He was sure that this organism was causing the cholera that had been ravaging the world since 1817, when it laid waste to Bengal. Its onslaught there was shocking, even for a region that had had cholera – or something similar – for so long that there was a specific cholera goddess, Ola Beebee (translated as ‘our Lady of the Flux’).
Ola Beebee was meant to protect against this mysterious affliction, which terrified people. Who would not be scared by seeing “the lips blue, the face haggard, the eyes hollow, the stomach sunk in, the limbs contracted and crumpled as if by fire”? Although 1817 is the official starting date of the first cholera pandemic, humans and cholera have almost certainly coexisted for far longer: that description of cholera’s distinct symptoms was inscribed on a temple in Gujarat, India, over 2,000 years ago.
The world is currently living through the seventh and longest cholera pandemic, which began in Indonesia in 1961 and, before Haiti, was most famous for an outbreak that devastated South America in 1991, killing 12,000 people in 21 countries.
People with access to clean water and sanitation probably think of cholera as being as old-fashioned as smallpox, and long gone. Surely the problem now is Ebola? Away from headlines, though, the gram-negative, rod-shaped bacillus Vibrio cholerae has been consistently murderous. It is currently present in 58 countries, infecting 3–5 million people a year and killing 100,000–120,000. This latest pandemic, wrote Edward T Ryan of Harvard University, “as opposed to burning out after 5-20 years as all previous pandemics have done…seems to be picking up speed.”
On 11 February this year, Johnson ate soup made from yams and bananas bought at the local market. By late afternoon, he was vomiting. With his soup he had swallowed Vibrio cholerae, which usually reach humans through contaminated food or water. Inside his body, the toxin secreted by the cholera bacteria bound to the cells in the wall of his small intestine, causing channels in the cells to stay open. Johnson’s disrupted cells flooded his gut with chloride ions. Sodium ions and water followed, causing his body to expel fluid and electrolytes and passing on more Vibrio bacteria to infect new hosts. A cholera victim can lose several litres of fluid within hours. Cholera can invade the body of a healthy person at daybreak and kill them by sundown.
Johnson is now safe and healthy in Jenniflore’s house, an hour away from his. He survived because he was taken to a nearby cholera treatment centre (CTC) run by Médecins Sans Frontieres (MSF) and because cholera, despite its power, is easy to treat. Eighty percent of cholera cases are cured by the administration of a simple oral rehydration solution.
Four hours’ drive from Port-au-Prince (it should be two, but it takes two hours to escape the city’s atrocious traffic), I get into a white four-wheel drive vehicle belonging to Action Contre La Faim, a French NGO that is a local implementing partner for UNICEF (one of the major actors in Haiti throughout the epidemic) and also the host of my trip. I’m nervous: this will be my first encounter with cholera patients, and with a CTC. What if the place stinks? How should I react? I don’t have long to think about this because the first visit is to the CTC in Gonaïves, the departmental capital, only a few minutes’ drive from the Action Contre La Faim compound.
It’s a small structure behind a blood bank, located in a yard near a toilet block that includes one stall marked ‘Cholera Patients’ and another marked ‘Tuberculosis’. Before I can enter, I must be chlorinated: hands, first, then I press my shoes onto a chlorine-soaked mat. (“Chlorine is our best friend,” I’m told in another CTC by a smiling clinic worker.) Inside, the small clinic is rudimentary but clean. There are four patients in the treatment area: a young man sitting on his bed, an older woman lying on hers, and two children, including five-year-old Junior*, whose eyes are shut and whose bottom is naked. He looks weak and sick, and it’s heartbreaking.
The ward doesn’t smell, although each patient is lying on a cholera cot, a special bed that has a hole cut out of the canvas and a bucket underneath to catch what in Creole is called dlo diri (from de l’eau de riz, ‘rice-water’), the watery diarrhoea that pours out of cholera patients. When I show images of these cots to friends, they are shocked. Such indignity! But there is no dignity when you are expelling dlo diri. A hole and a bucket are comforts, along with either oral rehydration solution or an IV drip with glucose and electrolytes. A patient’s precise treatment depends on whether they are classed as Plan A (observation and rehydration with oral rehydration solution), Plan B (rehydration and possibly an IV drip) or Plan C (definitely an IV drip).
Junior’s mother Mirlande* says her son was playing outside then started vomiting. She knows how cholera gets you: through dirt, touching people with cholera or not washing your hands. Junior is being treated with an IV drip and yesterday had felt better, but today he’s vomiting again. It’s good she brought him here. In recent years, cholera has become stigmatised. Recipients of cholera kits – soap, water-sterilising Aquatabs and, often, a bucket – are thought dirty. Some sufferers travel hours on motorbikes to get to a CTC far enough away that the neighbours don’t find out, and die en route. Although cholera is most deadly to small children, the elderly and the weak, this basic CTC has given Junior good care in good time and I am glad that he will probably survive. The trouble is, in 2015, the CTC shouldn’t be here at all.

Parkin Parkin
Cholera, it is often said, is a symptom of poverty. Cholera loves chaos. Haiti, home to both chaos and poverty, is a place where cholera thrives. Even before the 2010 earthquake, Haiti ranked 145th out of 169 countries in the United Nations' Human Development Index. It was the poorest country in the western hemisphere, and 70 percent of the population lived on less than $2 a day. In 2014, only 17 percent of the rural population had access to improved sanitation, and around 40 percent used unprotected water sources, including rivers. There is regular disaster, caused by corrupt governments such as the Duvaliers, or coups or hurricanes. The 2010 earthquake killed at least 220,000 people and left 1.3 million homeless, according to Haitian government figures (a 2011 USAID report estimated up to 85,000 deaths). By the middle of 2010, Haiti was dealing with a horrifying set of problems. But it didn’t have cholera, a disease that had not been seen on the island for 100 years.
A fellow resident of my guesthouse remembers eating in a restaurant in Artibonite (one of the ten administrative departments in Haiti) in autumn that year. “They brought out a fish. Then suddenly someone came and grabbed it. ‘Don’t eat that! People are dying. There’s something wrong with the river.’”
There was definitely something wrong with the river. The first recorded infections were in members of a family living in Meille, near the Artibonite River, probably on 14 October. Five days later, investigators found ten more cases in 16 surrounding houses. Also in Meille was a battalion of Nepalese peacekeepers working for MINUSTAH, the United Nations Stabilization Mission in Haiti. Rigorous investigation strongly suggests that the cholera came from sewage discharged by the base into the river. The cholera was Vibrio cholerae 01, serotype Ogawa, biotype El Tor, a strain never seen in Haiti, and confined until then to Asia and parts of Africa. This same strain of cholera had broken out in Kathmandu on 23 September 2010, shortly before the peacekeepers left for Haiti.
By the end of December, there had been 185,351 cases and 4,101 deaths. Haiti was in a state of terror. Nobody dared shake hands or touch, never mind eat the fish. There were so many corpses that sometimes people transported their dead relatives on a motorbike, propped up between two passengers. People turned to voodoo priests – houngans and mambos – then blamed them too, just as the residents of Britain attacked doctors and hospitals in 1832 after the ‘Asiatic cholera’ of Bengal had reached England via the port of Sunderland and a ship from Hamburg.
The lower classes rioted from Paisley to Dublin to London, convinced that cholera was a plot by the wealthy to do away with them, so targeted seemed this “scourge”. Fears of ‘burking’ – people being murdered for anatomical research, named after the infamous Burke and Hare – led to medical gentlemen being attacked in the streets. The new cholera hospital of Leeds was stoned; Liverpudlians had eight major street riots in two weeks. When a cholera hospital was opened in Toxteth, a mob of men, women and children joined in “hooting, screaming and assaulting several persons who endeavoured to explain the nature of the establishment”.
In fear there is room for superstition, and so it was in Haiti. But there was also a huge and admirable effort from government, NGOs and the UN in treatment and prevention. CTCs were established, as was hygiene messaging that reminded people to wash their hands before eating and after defecating to prevent the spread of dangerous faecal particles. Aid poured in.
By 2014, it was working. After the dreadful death tolls of 2010–12, disease spread and fatality were being cut by nearly half each year. There were 352,033 cases and 2,927 deaths in 2011, compared to 27,659 cases and 295 deaths in 2014 (although the number of cases in 2013 in Haiti was still more than the rest of the world’s put together).
“In 2014 we were close to eliminating cholera. We were really close,” says Gregory Bulit, the emergency manager for UNICEF. Of the 800 cases in the country, he says, only 50 percent tested positive for cholera. Include the 30 percent false-positive rate of the rapid diagnostic stool test and that number drops still further.
“From January to February,” says Oliver Schulz, head of MSF Haiti when I visited, “the number of cases was almost zero”. Even throughout the worst rainy season from April till June, which anyone working on cholera dreads (rain flushes out excreta from shoddy pit latrines, for one, spreading contamination), there had been no outbreak. The French epidemiologists Stanislas Rebaudet and Renaud Piarroux, who have done outstanding work in Haiti since the outbreak, called the reduction in cases “spectacular” [translated from French]. It looked as though cholera was about to be contained.
There was further cause for optimism. In 2013, the government launched a ten-year National Plan for the Elimination of Cholera in Haiti. It will require ten years because of the severity of Haiti’s infrastructural context (nearby Cuba, which has far superior healthcare and sanitation, has reported only 700 cases and three deaths, although its outbreak is ongoing). The targets are ambitious: by 2017, all public water systems will be regularly chlorinated and monitored. By 2022, Haiti’s water and sanitation access will be increased “to at least the average level of the countries of Latin America and the Caribbean”.
In 2014, the government announced a Total Sanitation Campaign, a joint water and sanitation initiative with the UN, because safely containing human excreta and supplying clean drinking water is as much part of the fight against cholera as oral rehydration solution. Nearly four million people, 2,500 schools and 500 health centres will be persuaded to abandon open defecation and use latrines.
A reorganisation of government in 2009 had already seen the creation of DINEPA, a water and sanitation agency that would oversee the improvement of sanitation standards. When cholera arrived, long-term development became an emergency response (which meant that DINEPA oversaw the chlorination of drinking water supplies). The cholera lull in 2014 saw the government begin an ambitious plan to turn the emergency response into a longer-term development plan overseen by the health ministry. NGOs would retreat. Agencies such as MSF began transferring CTCs to the government, and Haiti’s cholera status went from emergency to chronic.
Then came September. Suddenly, explosively, cholera resurged in Port-au-Prince. CTCs were reopened and quickly overwhelmed. When MSF – which had been considering closing its CTCs – opened a new clinic in Port-au-Prince, the first patient arrived within six hours. There were 1,834 cases in September, then 5,018 in October. Something had gone badly wrong.

Parkin Parkin
Up in the hills of Port-au-Prince, I accompany a team from one of UNICEF’s partner organisations, Croix-Rouge française (CRF). The capital spreads from these high hills down to the blue ocean, down to Cité Soleil, Haiti’s famous slum. Here in the hills is where cholera resurged, in the slum of Martissant, one of the poorest and most gang-infested areas of the city. CRF delivers emergency responses to outbreaks. If someone arrives at a CTC or clinic and is thought to have cholera, a team is dispatched – ideally within 48 hours – to set up a ‘cordon sanitaire’, or sanitary barrier. Speed is an important weapon, both in the spread of cholera and in the fight against it. UNICEF and other agencies are excited about a new Google Drive system that enables them to get real-time updates on cholera cases all over the country, something that didn’t exist before. If they know cholera’s routes, they can block them more effectively.
Today’s team wears red vests and baseball caps. They resemble the men on Port-au-Prince street corners who are selling mobile phone minutes, but they carry chlorine sprays, not phone cards. Our target is a narrow street. We reach it though other narrow streets, where women are selling raw meat and cooked food. None of it is covered. The flies are landing freely, their feet likely contaminated with faeces.
In the National Plan to Eliminate Cholera, the country’s sanitation is described as “practically non-existent”. Port-au-Prince has only one operational waste treatment centre for a city of two to three million people. People who do have latrines have them emptied manually by an underclass of bayakou (men who jump, often naked, into the pits and shovel out their contents). Hardly any of that shit is disposed of at the treatment plant; instead, it ends up anywhere the bayakou can put it. It’s the same ‘anywhere’ where the majority of Haitians without latrines go to do their open defecation. It’s the anywhere where cholera thrives.
We park, finally, and the team gets ready. One man is the disinfector. He puts on a mask, apron and gloves and gets his spray can. There are three stages of disinfection and three strengths of chlorine solution: today will be A-strength (four spoonfuls of chlorine solution in 20 litres of water) and the whole house will be sprayed, along with the neighbours’ houses. Another team member has a clipboard and pen. To combat the speed of contamination, questions are as important as chlorine. How did you get cholera? Where have you travelled? Who have you met? Cholera is easily transmitted in food and water, but also at funerals and carnivals and street markets.
The questions are being asked of Gaelle*, just discharged from a CTC after three days. She leans against the dingy curtain in the dingy concrete house as if it is holding her up. I ask her how she got cholera: “I don’t know. We treat our water.” She and her sister Lourdes* say they buy Aquatabs, water disinfection tablets that are widely available for sale but seen as expensive, unless they are dispensed freely by NGOs. (Most people add chlorine to their water, though usually too much.) I ask Gaelle how cholera is transmitted: “With dirty hands or when the environment is dirty.” Finally, in my most patronising mode, I ask what she thinks cholera is. A small animal, a virus? “No,” she says with some pity for my stupidity. “It’s a microbe.”
When I interview Haitian officials, they talk about outreach and messaging. They mean hygiene posters and pamphlets and megaphones that instruct Haitians to wash their hands, treat their water, keep themselves clean. I don’t think this kind of top-down didactic approach works ordinarily: no one responds well to hectoring. It’s even less successful when the messages are so well known, says one NGO worker, “that if you start [a sentence about hygiene], it’s them who finish the sentence.” As cholera retreated, lassitude grew. “They know what to do,” says Olivier Lamothe, who works on emergency responses for UNICEF. “They say, ‘but I’ve always done that and there was no cholera’. There’s a reticence. We have to figure out how to adjust the message.”
Many residents of Port-au-Prince get their water from official water points monitored by the government. Others buy it from kiosks with names like Eau Miracle (slogan: “I drink Miracle Water; do you?”). There are so many of these kiosks, I don’t see how they can all be monitored. Even if they were, gangs in Martissant have been breaking into the mains and trucking water up the hills, where the pipes don’t reach, to sell it. Breaking into a water main is a great way to get it contaminated, and it’s probably the reason why cholera broke out again in Martissant in 2014. “The network is permeable,” says Gregory Bulit. It’s so bad, official talks are going to be set up with the gangs. If they must sell the pirated water, then at least let it be pirated and chlorinated.
I look at Gaelle’s latrine, a dirty concrete pit inside her house, and wonder how a spray of chlorine can make it safe. I wonder how even all the effort and programmes can make everything safe: every food seller offering fly-covered pigs’ trotters, every hug of a corpse at a funeral and the dirt underneath every child’s fingernails. It seems so daunting. And it will cost a fortune: the government costed the National Plan for the Elimination of Cholera at $2.2 billion, and a high-level conference on Haiti at the World Bank last year estimated that $310 million would be needed over the next three years, plus $70 million more to fix Port-au-Prince’s water supply.
The money is of course lacking. UNICEF, government, MSF, anyone – whenever I ask about funding, I hear the same three words: Ebola, Syria, Ukraine. Donors have forgotten Haiti. Their heads have been turned by other, more dramatic causes. Drama attracts money; water mains and pit latrines do not.
Vibrio cholerae itself is a daunting adversary. About 75 percent of infected carriers show no symptoms but remain contagious for up to two weeks. Cholera, it’s now understood, can survive in aquatic environments, making it far harder to eradicate. Oliver Schulz of MSF calls it “predictably unpredictable”. Even so, he tells me, you can be prepared for the unpredictable. But in 2014 the Haitian government wasn’t. There was “a deplorable absence of an effective national (and departmental) response system”, as MSF’s latest Haiti cholera report put it.
When the outbreak surged in Martissant, it took days for information about confirmed cholera cases to be reported back. Local government was supposed to take on more responsibility, but local authorities took six weeks to notice that a treatment centre had been reopened in Cité Soleil. The outbreak could have been contained with better reaction times and better information gathering, but people’s attention was not where it should have been. “Preparatory activities for a hypothetical importation of Ebola diverted the attention of MSPP,” wrote the epidemiologists Stanislas Rebaudet and Renaud Piarroux in a report for UNICEF [translated from French]. By December, it was too late. In December, the only national laboratory in the country capable of doing microbiological diagnosis closed when an air-conditioner broke, a situation that the epidemiologists called “ubuesque” after the French absurdist play Ubu Roi. It was still shut in February.
There is more absurdity. On my way out of the Gonaïves clinic, I’d stopped at the nurses’ desk. Three women in nurses’ uniform were sitting squashed up on a bench. They looked miserable, and no wonder – they hadn’t been paid for 13 months. Outside a CTC in Gaumont, an hour’s drive away, the hygienist (who I had seen gathering up used syringes) stopped to chat. Jacob is 33 and has been working at the CTC since seven days after it opened in 2010; he was previously a mechanic but thought that working there was more important. In the worst times, he used to get a salary. Now he is paid an allowance by Action Contre La Faim, but only during outbreaks. Today is the last day of the outbreak: “Tomorrow, I will be a volunteer again.” But he will keep coming.
The government emergency health teams EMIRA – Équipes Mobiles d’Intervention Rapide – have been unpaid for months. At the time of my visit, there were nearly $2 million of unpaid salaries. I’m told of blockages in the Health Ministry and a top-down culture where the smallest expense must go through the minister. The unpaid workers stay at work, thankfully, because they are good people in a cholera epidemic or because they don’t want to lose their jobs. By April, there had been 14,226 new cholera cases, an increase of 306 percent on the year before. Twenty-one Haitians have died.
I ask people if they are optimistic. ‘With reservations,’ says Oliver Schulz of MSF, whose impressive CTC in Delmas 33 I visit on my way to the airport, so that I leave Haiti wafting chlorine. He says that cholera can be eliminated (reduced to zero cases in a specific area) but not eradicated (permanently reduced to zero cases, worldwide). “This is an island nation with a border. It is possible to contain it. Cholera is so crazy and so easy to treat.”
‘Yes,’ says the Elimination Plan, although an Action Contre La Faim official describes it as “tidied away on a shelf”, for all the good it has done so far.
‘Yes,’ says the President of Haiti, Michel Martelly, who told Time that he has tried “to change the perception of Haiti as a place where nothing works”.
‘Yes,’ says the brand new Marriott Hotel, opened during my visit, which is meant to symbolise Haiti’s fast-growing economy and faces the hills where people drink Vibrio cholerae.
‘No,’ says a chief nurse in the hospital at Gaumont, which houses a CTC. No, because only three of her nursing staff are paid, yet they are expected to cover the whole hospital and the CTC, as well as report data promptly. She is furious. “We can’t eradicate cholera. We’ve no clean drinking water, there are no toilets. We are not going to escape this.”
*Names have been changed
This article first appeared on Mosaic in July 2015.
- Final Report of the Independent Panel of UN experts on the Cholera Outbreak in Haiti, a lucid view at how and why the cholera came back to Haiti after 200 years.
- Ryan ET PLoS Negl Trop Dis 5(1):e1003 (2011) The Cholera Pandemic, Still with Us after Half a Century: Time to Rethink, a really clear more global overview of why we're still being assaulted by a pandemic that began in 1961.
- Piarroux R et al. Emerg Infect Dis 17:7 (2011) Understanding the cholera epidemic, Haiti. Rene Piarroux has done peerless research into Haiti's cholera outbreak, along with his fellow epidemiologist Stanislas Rebaudet
- Marisa C. Eisenberg et al. Epidemics 5(4):197–207 (2013) Examining rainfall and cholera dynamics in Haiti using statistical and dynamic modeling approaches. Quite technical but a fascinating look at the correlation between weather and disease.
- Haiti: Clean water, improved sanitation, better health: Haiti Conference, Washington DC, 2014. Report of a high-level conference into Haiti held at Washington DC, with good overview and prospects for the future.
- The biology behind cholera: from Big Picture, the Wellcome Trust's educational website.
- Desperate love in a time of cholera: Exploring the struggle between love and disgust when caring for sick relatives, from elsewhere on the Mosaic site.
- Cholera & Conflict: 19th Century Cholera in Britain and its Social Consequences. Edited by Michael Holland, Geoffrey Gill and Sean Burrell. Thackray Museum, 1999. Most books about the cholera in 19th century Britain focus on the (admittedly wonderful) John Snow. This book looks at other cities where cholera also thrived, even though London got, and gets, most of the attention.
- The Ghost Map by Steven Johnson. This is the best most recent narration of the story of John Snow and how he mapped cholera in London.
- Institute of Justice and Democracy in Haiti. A really comprehensive site for all sorts of news on Haiti, with a clear and detailed set of references and resources relating to cholera and the attempts to get reparation for its victims.
- Sustainable Organic Livelihoods Haiti (SOIL): an NGO that is trying to improve the sanitation situation in Port-au-Prince and Cap-Haitien regions, by promoting ecological sanitation. Dry toilets, composting of human "waste" and the selling of "konpo lakay" (local compost). Sustainable sanitation, sustainable social business: SOIL are doing great things.

